This is the place for you to find answers to frequently asked questions about respiratory syncytial virus (RSV).
How Does RSV Spread and Who Is Most at Risk?
How can my baby get RSV?
RSV is easily spread through coughs, sneezes, and close physical contact, like cuddles and kisses.1,2
An RSV infection can cause mild, cold-like symptoms,1 but most people may not realize they're infected with RSV and may spread the virus to others.3 Research has shown that RSV is mostly spread to babies by older siblings or other children.4,5
RSV can also survive on soft surfaces, such as clothing and fabrics, as well as hard surfaces, such as toys and utensils, for many hours. It can then spread to babies if they touch the infected surface and then touch their eyes, nose, or mouth.1,2
What age group does RSV disease affect?
RSV can affect people of all ages, but it can be particularly severe in babies and older adults.8
Among every 10 babies infected with RSV, 4 may develop severe lung infections such as bronchiolitis or pneumonia.9
Does Hong Kong have obvious RSV seasonality?
RSV infections occur throughout the year in Hong Kong and are highly transmissible.10
RSV Severity and Complications
Is RSV serious for infants?
RSV usually causes mild illness but, in some babies, it can become severe within just a few days,6 potentially leading to lung infections such as bronchiolitis or pneumonia.1 These infections can cause swelling in the airways, which may make it harder for babies to breathe.7
Signs that a baby is struggling to breathe can include wheezing, grunting, or breathing faster than usual.*7
All Infants are at Risk of RSV Infection
2 out of every 3 infants will be infected with RSV before their first birthday.11
90% of children will have had an RSV infection by age 2.11
1 in 5 children under age 2 will require outpatient care due to RSV.12
1 in 50 infants will be hospitalized within their first year of life due to RSV.13
* Please note: this is not a complete list, other symptoms can occur and infants may not experience all of these symptoms. Other infections may also cause similar symptoms. When you are concerned about your child's health, seek medical advice.
Can RSV cause long-term complications in infants?
Studies show that after RSV infection, the most common short-term complications in children are Acute Otitis Media (middle ear infection)14 and Pneumonia14
Infants who are reinfected with RSV may face significantly higher risks:
- 7.7 times higher risk of hospitalization15
- 9 times higher risk of pediatric intensive care (PICU) admission15
- 4.5 times higher chance of recurrent wheezing, which may persist for over 10 years15
In addition, for healthy full-term infants who were not infected with RSV during their first year of life have a 26% lower risk of developing childhood asthma later on compared to those who were infected.16 This highlights the importance of early RSV protection.
Why RSV can cause Pneumonia or Bronchiolitis in babies?
Bronchiolitis is an illness caused by an infection in the smallest airways of the lungs, which are called bronchioles.1 When bronchioles become inflamed and swell, mucus can build up and block them, making it difficult to breathe.2
Some babies may develop pneumonia when RSV goes deep into their lungs, causing inflammation.7,17,18 This leads to fluid and pus building up in the tiny air sacs in their lungs, making it difficult and painful for them to breathe.7,17,18
Why it's important to protect babies under 1 year old from RSV?
2 out of every 3 babies will get infected before their first birthday.19
During their first year of life, babies’ lungs and immune systems are still developing, which makes them vulnerable to RSV disease. As a result, infants face a higher risk of severe RSV complications and hospitalization.20-23
During this vulnerable stage, babies are too young to develop enough effective antibodies against RSV. By giving them passive immunization, we provide effective antibodies that act like a temporary bodyguard, shielding them from RSV while their immune system continues to develop. 15,24-25
High-Risk Groups for RSV: Preterm, Full-Term, and Previously Infected Infants
Is there a higher risk of RSV if my baby is born early?
Infants born prematurely (before 37 weeks of pregnancy) are at higher risk of serious RSV infection than those born at term (37 weeks of pregnancy or more).26
If you are concerned, speak to your healthcare provider.
Can healthy full-term babies get RSV?
Even healthy, full-term babies are at risk of RSV infection.1
In fact, 9 out of 10 children will be infected with RSV by the age of 2.11 While most RSV cases are mild, symptoms can worsen rapidly within just a few days.6
Studies show that around 40% of babies infected with RSV may develop bronchiolitis or pneumonia.5 Surprisingly, over 70% of babies hospitalized due to RSV are healthy and born full-term.12 This highlights that serious complications can occur even in babies without underlying health conditions.
Although babies born prematurely or with chronic illnesses are considered high-risk, it’s impossible to predict which healthy infants might require hospitalization.27 That’s why RSV protection is important for all babies including those born full-term and healthy.
Can my baby get RSV more than once?
Yes, babies who have had RSV once are not immune for life. They can be re-infected, and studies show that the risk of developing serious respiratory illness increases with subsequent infections.15
RSV Care Advice for Parents and Caregivers
Is there a treatment for RSV disease?
There are currently no specific treatments for RSV, and it is generally managed with supportive care and symptom relief.1,3,31 Most cases are mild¹ and recover within a week or two.31 But in severe cases, treatment may include oxygen, feeding support, and hydration.1,32
What can I do to relieve my baby’s RSV-related symptoms?
Most RSV infections resolve on their own within one to two weeks. However, RSV can cause serious illness in some infants.31 If your child shows signs of difficulty breathing, poor fluid intake, or severe symptoms, contact your pediatrician or family doctor immediately.
Can a newborn regulate their temperature if they get a fever from RSV?
Babies are unable to regulate their body temperature in the same way adults can. It is very important for them to maintain a stable body temperature, particularly if they are born premature or are sick.33
Babies with RSV can experience high temperatures or fever.34 Consult your pediatrician or family doctor for more guidance.
How to help protect babies against RSV?
Maintain good personal and environmental hygiene10
Passive immunization: Preventative antibodies are an option available for protection against RSV in Babies10
Speak with your healthcare providers to learn more about RSV prevention options.

RSV vs Other Respiratory Infections
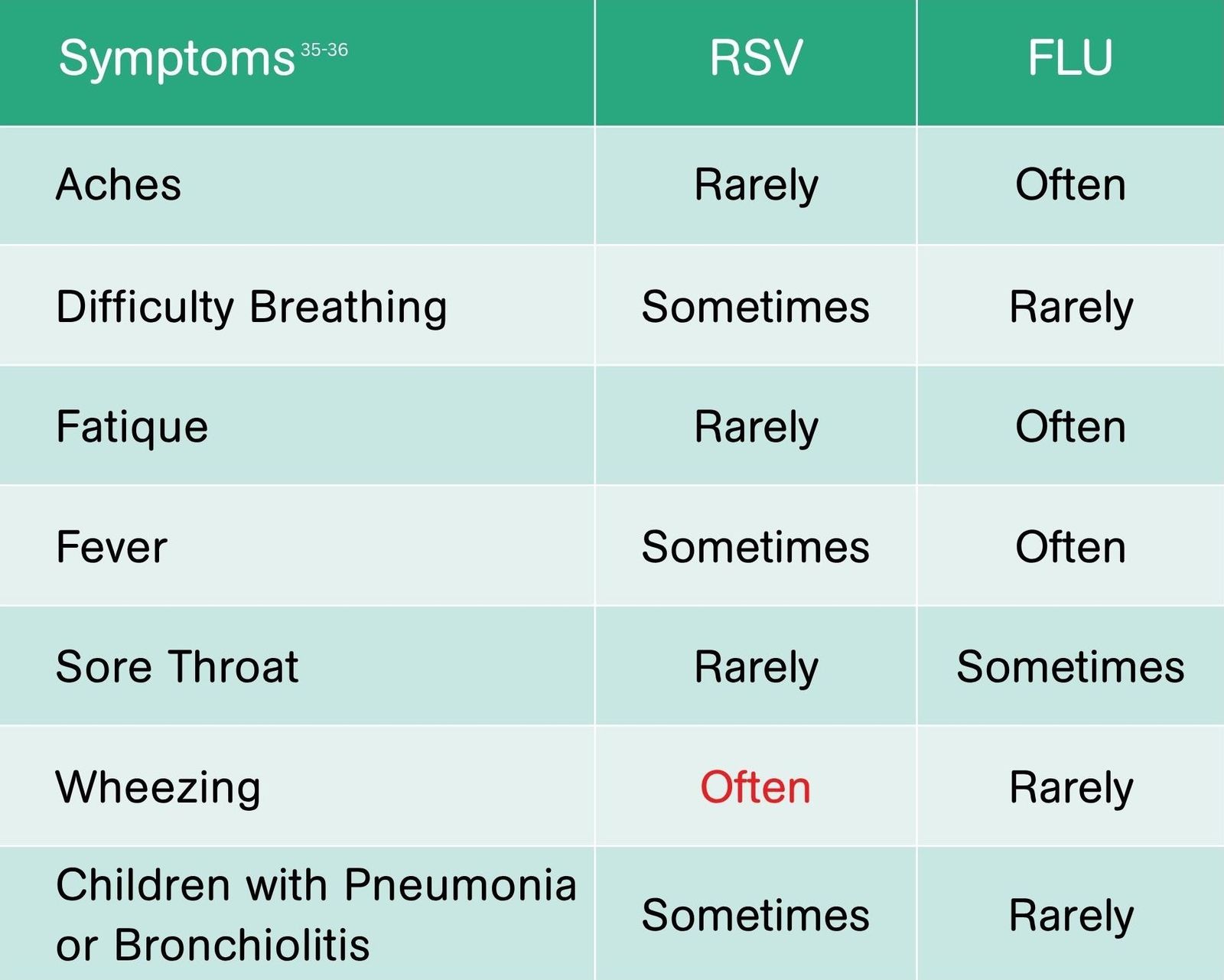
What’s the difference between RSV and influenza?
RSV and influenza are both contagious respiratory illnesses but they are caused by different viruses. While their symptoms such as coughing, fever, and difficulty breathing may appear similar, the impact on infants can be significantly different.
Compared to influenza and rotavirus, RSV poses a much higher risk of severe illness in babies under 1 year old:
Mortality rate: 10 times higher than influenza28
Hospitalization rate:
16 times higher than influenza29
2 times higher than rotavirus30
These statistics highlight that RSV poses serious threat to infants, especially those with immature immune systems. As a result, early awareness and prevention are crucial to protecting vulnerable young infants
Footnotes & references
RSV, respiratory syncytial virus.
1. Piedimonte G and Perez MK. Pediatr Rev 2014; 35(12): 519–530.
2. Centers for Disease Control and Prevention (CDC). How RSV Spreads. Available at: https://www.cdc.gov/rsv/causes/index.html (Accessed: July 2025).
3. Kaler J et al. Cureus 2023; 15: e36342.
4. Jacoby P et al. Epidemiol Infec 2017; 145(2): 266–271.
5. Yamin D et al. PNAS 2016; 113(46): 13239–13244.
6. Smyth RL and Breary SP. Encyclopedia of Respiratory Medicine. Bronchiolitis, Elsevier Ltd. 2006.
7. Meissner HC. N Engl J Med 2016; 374(1): 62–72.
8. Du Y et al. Int J Infect Dis 2023; 135: 70–76.
9. Piedi-monte G. Curr Opin Pediatr 2013; 25(3): 344–349.
10. Centre for Health Protection (DoH HK). Respiratory Syncytial Virus Infection 2025. Available at https://www.chp.gov.hk/en/healthtopics/content/24/36.html (Accessed: July 2025)
11. Lively JY, et al. J Pediatric Infect Dis Soc. 2019;8(3):284-286.
12. McLaughlin, et al. JID, 2020;jiaa752.
13. Sanchez-Luna M et al. Curr Med Res opin 2016; 32(4):693-698.
14. Abreo A, et al. Clin Infect Dis. 2020;71(1):211-214.
15. Custovic A et al. Pediatr Allergy Immunol. 2024 Jun;35(6):e14169.
16. Rosas-Salazar C, ChirkovaT, et al. Respiratory syncytial virus infection during infancy and asthma during childhood in the USA (INSPIRE): a population-based, prospective birth cohort study. Lancet. 2023;401(10389):1669-1680.
17. Mayo Clinic. Respiratory syncytial virus. Available at: https://www.mayoclinic.org/diseases-conditions/respiratory-syncytial-virus/symptoms-causes/syc-20353098 (Accessed: July 2025).
18. National Heart, Lung and Blood Institute. What is Pneumonia? Available at: https://www.nhlbi.nih.gov/health/pneumonia (Accessed: July 2025).
19. Walsh E. Clin Chest Med 2017; 38(1): 29–36.
20. McLaughlin JM et al. J Infect Dis 2022; 225(6):1100-1111.
21. Yu J et al. Emerg Infect Dis 2019;25(6):1127-1135.
22. Pickles RJ and DeVincenzo JP. H pathol 2015; 235(2): 266-276.
23. Simon AK et al. Proc Biol Sci 2015; 282(1821):20143085.
24. Verwey C and Madhi SA. BioDrugs 2023; 37:295-309.
25. Lambert L et al. Front Immunol 2014; 5:466.
26. Stein R et al. Pediatr Pulmonol 2017; 52: 556–569.
27. Hall CB et al. Pediatrics 2013; 132(2): e341–e348.
28. Thompson WW, et al. JAMA. 2003; 289(2):179-186.
29. Zhou H, et al. Clin Infect Dis. 2012; 54(10):1427-1436.
30. Nelson EA, Tam JS, Bresee JS, et al. J Infect Dis. 2005;192 Suppl 1:S71-S79. doi:10.1086/431492.
31. Centers for Disease Control and Prevention (CDC). RSV in Infants and Young Children. Available at: https://www.cdc.gov/rsv/infants-young-children/index.html (Accessed: July 2025).
32. Barr R et al. Ther Adv Infect Dis 2019; 6: 1–9.
33. NHS South Tees Hospitals. Temperature control. Available at: https://www.southtees.nhs.uk/services/children-and-young-people/speciality/neonatal/family-guide/temperature-control/ (Accessed: July 2025).
34. Smith DK et al. Am Fam Physician 2017; 95(2): 94–99.
35. National Foundation for Infectious Diseases. How to tell the difference between flu, RSV, COVID-19, and the common cold. Available at https://www.nfid.org/is-it-flu-covid-19-or-rsv-how-to-tell-the-difference/ (Accessed July 2025).
36. Erickson EN, et al. Pediatric bronchiolitis. StatPearls. Treasure Island (FL): StatPearls Publishing. 2025.

