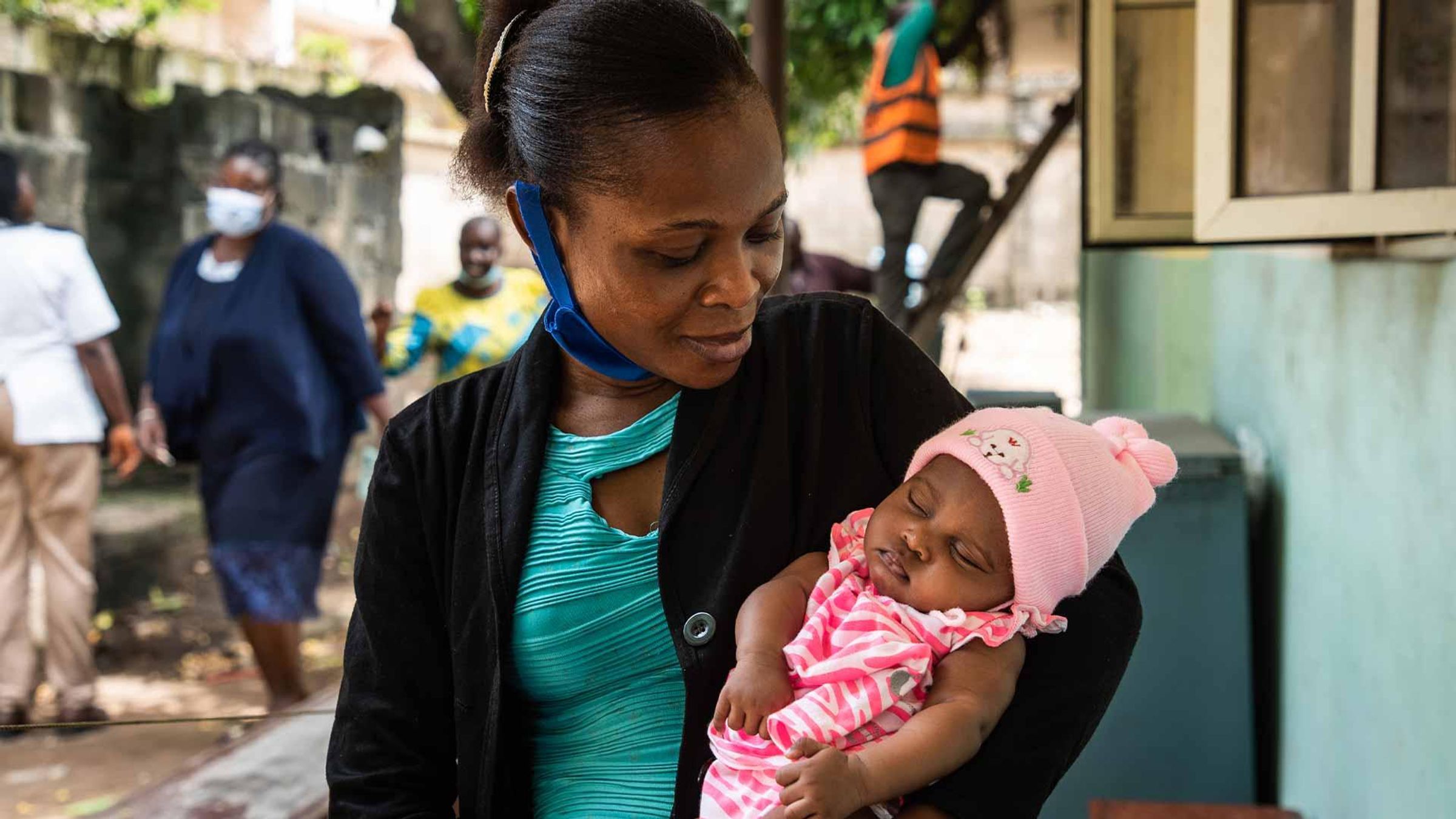
Poliovirus: Infection to Disease
01
1. Global Polio Eradication Initiative. Polio + Prevention. Available at: https://polioeradication.org/polio-today/polio-prevention/. Last accessed July 2021.
2. Mayo Clinic. Polio. Available at: https://www.mayoclinic.org/diseases-conditions/polio/symptoms-causes/syc-20376512. Last accessed July 2021.
The Fight Against Polio is Not Over
Healthcare workers, patients, and researchers are taking on polio.
1%
90%
In others,
Unfortunately, there is no treatment for polio.
Sources: WHO Introduction to Poliomyelitis and the Global Polio Eradication Initiative
Polio Introduction - WHO factsheet updated on July 22nd 2019
https://www.who.int/news-room/fact-sheets/detail/poliomyelitis and https://polioeradication.org/about-polio/
Three Serotypes of Wild Poliovirus
Immunity to one serotype does not confer immunity to the other two
type1.
type2.
type3.

The Story of Cosmos Okoli
Cosmos Okoli was diagnosed with polio at the age of four and had to crawl for seven years before he was able to get help. He shares his story and his fight against the disease.
Did You Know?
Poliomyelitis mainly affects children under 5 years of age
More than 18 million people have been saved from paralysis as a result of the global effort to eradicate the disease
Among those paralyzed, 5% to 10% die when their respiratory muscles become immobilized
Factors That Influence Poliovirus Transmission
Individual immune system
Weak routine immunization systems
Hygiene habits, sanitation and water quality
Densely populated communities
Explore more

Asthma and Whooping Cough don’t Mix
References
- WHO. Fact sheet N°114. Updated July 2019. Accessed September 2020. Retrieved from: https://www.who.int/en/news-room/fact-sheets/detail/poliomyelitis
- Polio Eradication. Accessed September 2020. Retrieved from: https://polioeradication.org/who-we-are/our-mission/
MAT-GLB-2104690 v1 – 10/2021
This page last update: 10-2021