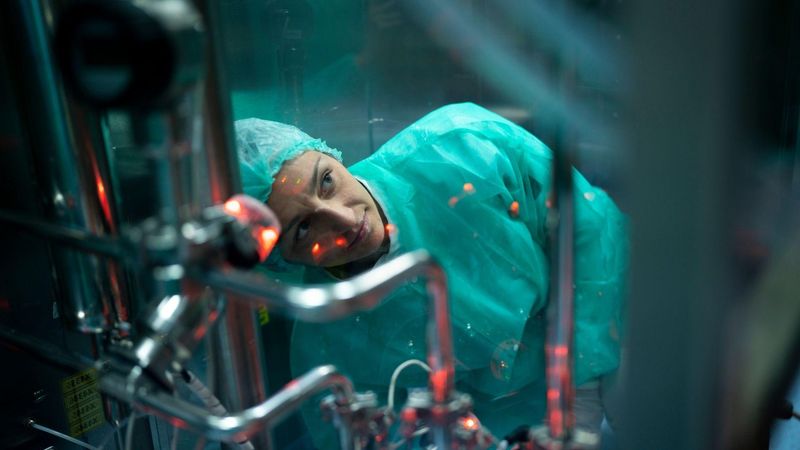
We’re an emerging leader in immunology, poised to transform medicine by rebalancing the immune responses that cause systemic, chronic diseases.
Our Immunology Pipeline
Our teams use real-world, molecular, and clinical data to advance precision medicine, and investigate:
- pathways common to systemic diseases like asthma and atopic dermatitis
- peripheral inflammatory diseases like rheumatoid arthritis
- autoimmune challenges in type 1 diabetes and cancer
Follow the Science
Taking Down Type 2 Inflammatory Disease
We’re working to tame over-active immune responses that drive systemic, chronic diseases.

From Wearables to Invisibles: Studying Sleep
Using AI and wireless tech, we’re helping people participate in research from home.
REGAINing Control of Asthma
We’re leveraging smart devices to understand the patient experience.
Type 2 Inflammation
Our goal: to give people their lives back by calming excessive inflammation–without compromising their ability to fight infection.
With our partner Regeneron, we study how blocking two interleukins1 can help calm type 2 inflammation, a driver of atopic dermatitis, asthma, chronic rhinosinusitis with nasal polyps, eosinophilic esophagitis, and other conditions.
Beyond Type 2 Inflammation
Precision Immunology
Single-cell genomics, genetics, and proteomics help us understand exactly what makes patients different from one another.
Checkpoint Immunology
How can we restore the delicate balance between a protective immune response and destructive autoimmunity?2
Complement System
Can we stop a cascade of inflammation without compromising immunity, by blocking one protein?3
Our Latest Science Stories
April 20, 2026
Shape Matters: Inside Molecular Clamp Vaccines
More for Healthcare Professionals
Our Data-sharing Commitments
Our Disclosure Commitments
Find a Clinical Trial
Campus Sanofi
References
- Mifflin L, Ofengeim D, Yuan J (2020) Nat Rev Drug Discov 19:553-571; DOI: 10.1038/s41573-020-0071-y
- Calabrese LH, et al. (2020) J Autoimmun 115:102546; DOI: 10.1016/j.jaut.2020.102546
- Nikitin PA, et al. (2019) J Immunol 202:1200-1209; DOI: 10.4049/jimmunol.1800998